Case for iPhone – IBOOLO
People May Ask
Moles exhibiting hues of blue, gray, red, black, or pure white could potentially indicate the presence of melanoma. D = Dimension: Moles exceeding a size of 6 millimeters, approximately akin to the eraser tip of a standard pencil, often evoke greater concern. (It is noteworthy, however, that melanomas can also manifest in minute, pinpoint-sized forms.)
Removing fresh ink stains is more straightforward when tackled prior to their drying and penetration into the fabric's fibers. It's crucial to dab away the excess stain meticulously, ensuring not to aggravate the issue by pressing it deeper into the material. To facilitate the subsequent cleaning process, consider utilizing rubbing alcohol, hairspray, or even hand sanitizer as an effective agent to weaken the stain's hold, thereby simplifying its removal during laundering.
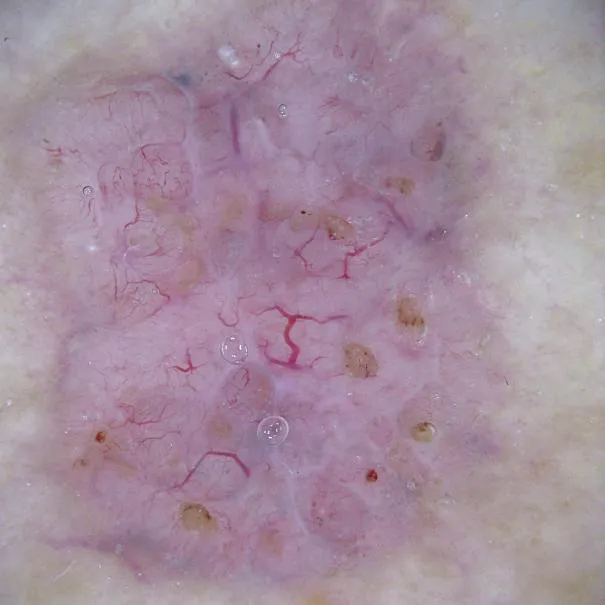
A lentigo is characterized as a pigmented lesion, either flat or mildly elevated, featuring a distinctively outlined border. Contrary to an ephelis, it maintains its color throughout the winter season. There exist numerous variations of lentigo. The term lentigo initially gained its name due to its resemblance to the appearance of a tiny lentil.
Two characteristic attributes often associated with melanoma in situ, specifically the presence of asymmetrical dots or globules and unevenly shaped streaks, are typically absent in ink spot lentigo cases. However, if these features are noticed, they ought to be regarded with caution and considered suspicious.
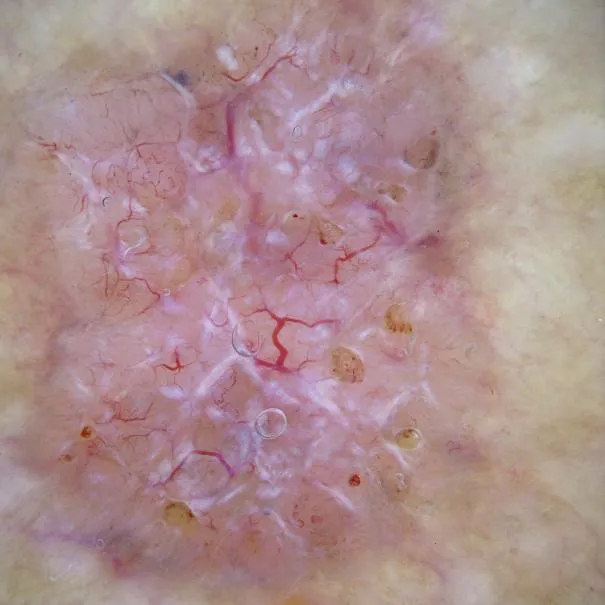
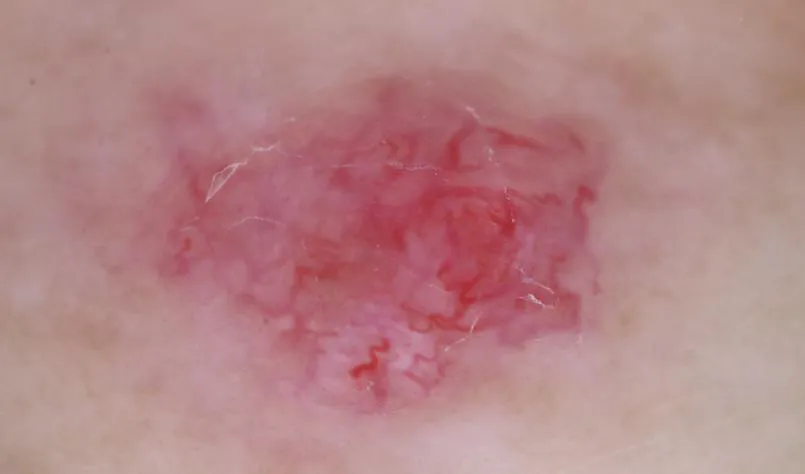
Clinically, lentigo maligna manifests as a visibly pigmented, irregularly shaped spot that initially arises on the cranial and cervical regions, progressing with a gradual expansion. The most favored approach for confirming the diagnosis of lentigo maligna entails performing an excisional biopsy. Upon histological examination, it reveals an increased number of abnormal melanocytes congregating in small clusters or isolated cells at the junction where the epidermis meets the dermis.
Documented recurrence frequencies range from 6% up to 20%, subsequent to extensive local excision (ELE) procedures, adhering to the guideline-prescribed surgical margins of 5 millimeters for melanoma that is confined to the skin's surface. January 18th, 2023.
It has been documented that approximately 3 to 10 percent of cases witness the emergence of invasive melanoma originating from lentigo maligna.
For many individuals, ablative therapy with cryotherapy is often perceived as the primary treatment choice for solar lentigines. The efficacy of this approach stems primarily from the sensitivity of melanocytes to the freezing effect of liquid nitrogen. Specifically, melanocytes are susceptible to freezing temperatures ranging from -4 to -7°C, whereas squamous cells exhibit resistance to damage even at -20°C.