Case for iPhone – IBOOLO
People May Ask
The differential diagnosis pertaining to the herald patch encompasses conditions such as tinea corporis, nummular eczema, along with erythema annulare centrifugum, as of February 15, 2024.
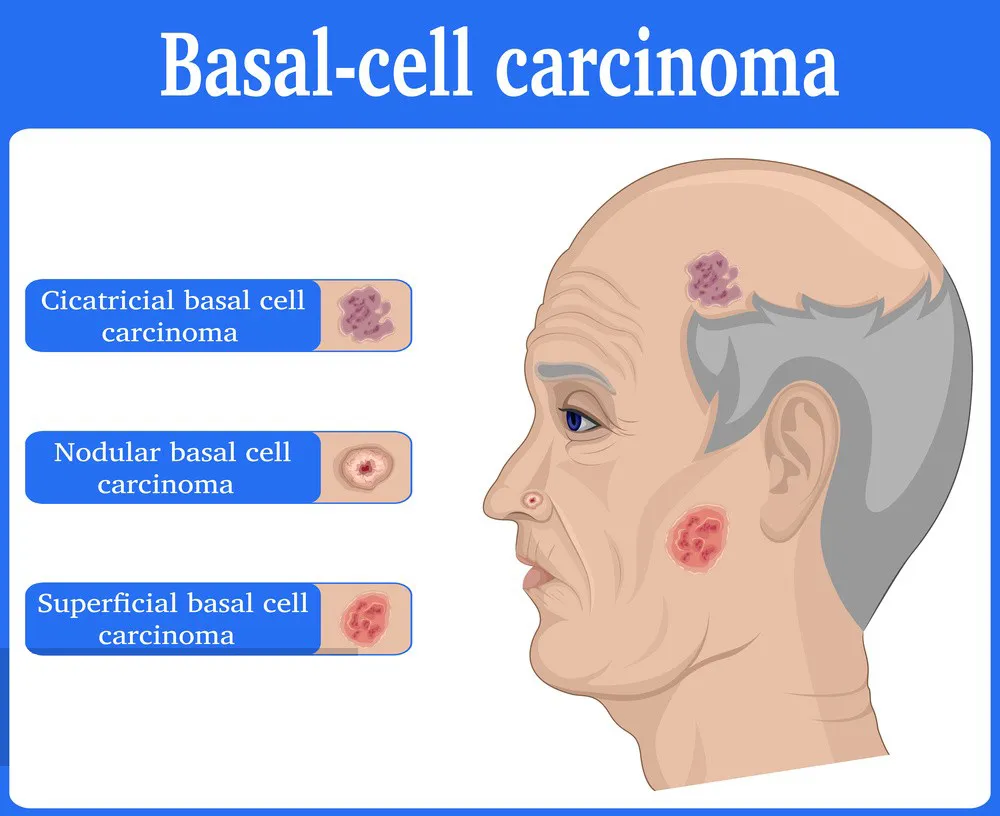
The majority of squamous cell carcinomas affecting the skin are attributed to excessive exposure to ultraviolet (UV) radiation. This UV radiation can originate from natural sources such as the sun, as well as artificial sources like tanning beds and lamps. Safeguarding your skin against UV light is an effective means of mitigating the potential for developing squamous cell carcinoma of the skin and various other types of skin cancer.
In the absence of conclusive evidence from imaging examinations that exclude the presence of sarcoma, it is imperative to conduct a biopsy prior to embarking on any therapeutic interventions. This step is crucial for establishing the diagnosis of sarcoma, whether it involves bone lesions, soft tissue nodules, or protrusions, and further pinpointing the specific subtype. Additionally, a biopsy offers valuable insights into the potential rate of cancer growth and dissemination.
The comprehensive understanding of the origins of generalised eruptive keratoacanthomas remains elusive, yet they have been implicated in various factors, including the involvement of Human papillomavirus infection, albeit without definitive evidence of consistent correlation or causation. Additionally, ultraviolet radiation has been considered a potential contributor, considering the proclivity of these lesions to manifest on skin areas frequently exposed to sunlight.
At times, it may be challenging to distinguish between pityriasis versicolor and vitiligo due to their shared attribute of producing uneven skin pigmentation in the form of patches.
Despite its general classification as a benign epidermal tumor, there have been infrequent instances of Clear Cell Acanthoma (CCA) exhibiting malignant characteristics. 20th October, 2022
The occurrence of clear cell carcinoma is commonly linked with endometriosis, clear cell adenofibromas, as well as atypical proliferative (borderline) tumors of the clear cell type, yet conclusive molecular proof supporting a gradual progression model remains elusive.
Seborrheic keratoses represent a skin condition characterized by the development of wart-resembling outgrowths. These growths possess a non-malignant (benign) nature, frequently leading to misidentification as nevi due to their inflammatory and erythematous appearance. As a therapeutic approach, the application of liquid nitrogen is commonly advised for managing these conditions.
Sarcomas might be erroneously identified as an abscess, a collection of blood within tissues (hematoma), or a benign fatty mass.
Acanthoma of the skin cells, though infrequent, is a benign tumor of epithelial origin with an uncertain cause. Clinically, it is evident as a papular-nodular formation or a minute, rounded, erythematous patch on the lower extremities of middle-aged individuals.